The gland you left behind
What your prostate did when it was doing what it was supposed to be doing

If you've never quite wrapped your mind around your greatest existential threat, illustrations like this may be why:

Considering what your prostate has gotten you into, you owe this much to yourself: a walnut-sized tour of the walnut-sized gland.
Plumbing
You probably already know the prostate is partly a valve, selecting urine or semen to exit the penis. Replacing two tubes with one1 sounds like a dubious feature, but prostates originated in the early mammals and today nearly every male mammal has one. We do possess a rare claim to prostate cancer, which ordinarily affects only rats, dogs, and men.2
With valves in mind, consider the first image of the nifty illustration below. At the bulge below the purple sphere3, the semen plumbing (blue) and the urine plumbing (yellow) converge.

For now we’ll think of the prostate as a single organ, but we see clearly here how it’s built of three roughly concentric zones, which we’ll revisit.
On-ramps
The prostate is a urinary highway with two on-ramps. The through route is the urethra coming from the bladder on top and exiting at the bottom.

First on-ramp: The many prostatic ducts carrying the prostate’s glandular contribution.
Second on-ramp: The two ejaculatory ducts — outlets of the seminal glands (or seminal vesicles) drawn in blue earlier — opening on an inner bulge called the verumontanum.
That third verumontanum opening, the prostatic utricle, is “blind” — it goes nowhere. If you’d developed into a female in the womb, it would have become your vagina.
Juice
The prostate’s glandular job is to secrete prostatic fluid, which makes up 25% of semen.4
The biggest contribution to semen — 65% — is from the seminal vesicles.
Sperm itself makes up just 10%.
In the prostate, all three mingle.
Precum (I had to look up the polite name — pre-ejaculate) it turns out is none of these; it’s secreted by two pea-sized organs downstream from the walnut-sized one. These glands — Cowper’s glands (or bulbourethral glands) — contribute a tiny fraction of semen.
The seminal fluids give sperm mobility, energy, antioxidants, a proper pH, and more. The non-sperm contribution to semen is called seminal plasma.
So let’s hook up your reproductive tract:

The connection between testicles and prostate is the vas deferens, a pair of 18-inch tubes starting in back of the testicle, looping over the top of the bladder, and widening just before the prostate into a bulge, the ampulla, that serves as a reservoir for sperm. At the ampulla each vas deferens is joined by the 2-inch-long seminal vesicle.
Why your pad is wet and your orgasm is dry
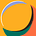
You, with the CVS bag of Depends, may remember being told there are two urinary sphincters, voluntary and involuntary, and that prostatectomy puts the involuntary sphincter at risk.
The involuntary sphincter is what closes during sexual arousal so semen doesn’t go up into the bladder and urine doesn’t go down out the penis.
It lies at the bladder neck where the prostate begins. If your bladder neck is short, prostatectomy is bad news for the sphincter.
Dry orgasm
Post-prostatectomy orgasms are dry because the organs creating seminal plasma are gone. The vas deferens, since it has nothing to connect to, is tied off, so there’s no sperm either. The sperm in the testicles gets broken down and reabsorbed by the body — just as if you’d had a vasectomy or had been sexually abstinent.
Prostate contractions participate in ejaculation, but they’re not doing the spurts. Ejaculation has two phases: In emission, prostate contractions flood semen toward the penis — progression to climax feels (and is) unstoppable. In ejaculation, muscles at the base of the penis contract repeatedly to spurt out semen.
Prostatectomy can make orgasm a hollow experience because the organ contributing the nearing-the-edge excitement is gone.
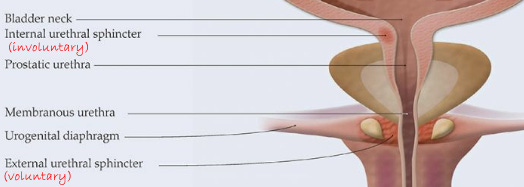
Nerve-sparing surgery
Cutting through the urethra, as surgeons once did, severs the nerves that control erections. To preserve the nerves, the cut has to stop short and nerves clinging to the prostate need to be peeled off.
As you may have read, even nerve-sparing surgery is traumatic, and erections can take more than a year to return.
Up and down
In anatomy texts, the apex (top) of the prostate is its downstream, penis-facing side, and the base is the upstream, bladder-facing side — the opposite of what you might think.
Prostate zones
To conclude the tour, let’s revisit the Russian doll we started with. Knowing the zones is like having a map with state outlines.
Digital rectal exams probe the peripheral zone, as you are now knowledgeable enough to verify.
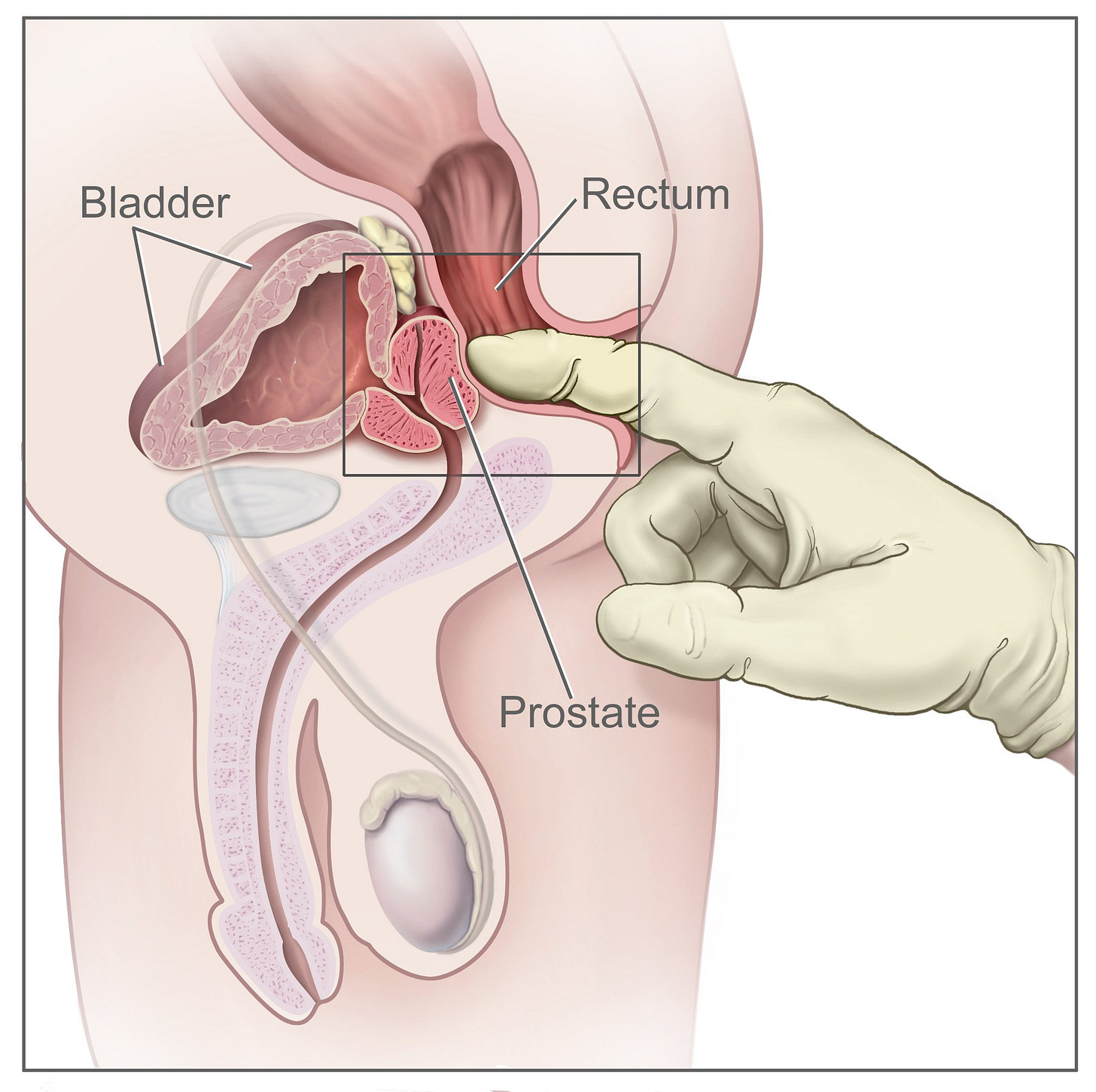
The peripheral zone, which occupies 70% percent of the prostate, is where more than 80% of cancers start, so it’s good that that’s what gets fingered.
The transition zone grows with age and is where BPH occurs. About 10% of cancers begin here.

The central zone, comprising 25% of prostate volume, is where roughly 5% of cancers (largely bad ones) start.
Now that you’ve taken the trouble to learn zonal geography, you probably won’t find zones in your pathology report. Current treatment is “zone-agnostic.” That overlooks the zones’ differences at the microscopic and molecular levels and their different prognoses, and a 2021 paper argues, “The unique biology of each zonal tumor type could help to guide individualized treatment and patient risk stratification.”
The anterior fibromuscular stroma5 (the last layer) wraps the front of the prostate and is purely structural.6
Birds, with a cloaca, go three-in-one.
Mice used in prostate cancer testing need to be genetically altered.
We’ll revisit that bulge. It has an interesting past.
The prostate, like a sweat gland, is an exocrine gland — it secretes into a duct. Endocrine glands, a term you’ve probably heard, secrete into the bloodstream.
Anterior is front; the more familiar opposite is posterior. Stroma is structural or connective tissue.
Cancer in this tissue would be rare and different from what we usually think of as prostate cancer.

Ben,
This was a great, comprehensive, easy to understand discussion about the prostate and its function! I have been missing mine for 14 years and it was a pleasant, yet wistful trip down memory lane. I should have asked for mine in a jar so I could look at it now and again to remind me of better times.
Richard
Hi Ben,
This is a very helpful and informative post. I intend to forward it along to some friends who have become PCa fellow warriors. I’m sitting in my lodging in Philadelphia a few days into what looks to be thirty-seven sessions of proton beam treatments (PBT) following biochemical recurrence (BCR) after three years post radical prostatectomy (RP) during which time I watched my quarterly PSA test results rise from undetectable to .21 thus beginning BCR. Now, I’m into radiation treatment (RT) of my prostate bed and lymph nodes using PBT at the Roberts PB Center at the University of PA. It is an amazing facility and is reported to be the largest PBT facility in the USA doing treatments five days each week from 7:00 AM to 7:00 PM = 300 procedures each week. Very impressive if you need BCR RT! Take care JPD